Perimenopause Headaches: Why They Happen and How to Support Your Body Gently
If you’ve started noticing more headaches or migraines than you used to, especially around your cycle, you’re not imagining it.
For many women, headaches are one of the earliest and most confusing signs of perimenopause, often showing up years before periods become irregular or other symptoms start.
The good news?
Perimenopause headaches are not random. And they do not have to be permanent, either. They’re signals and when we understand what’s happening underneath, we can support the body in ways that truly help.
What Is Perimenopause, Really?
Perimenopause is the transition phase leading up to menopause. It can begin as early as the mid-to-late 30s, rarely even in the late 20’s, and often lasts 8–10 years.
During this time:
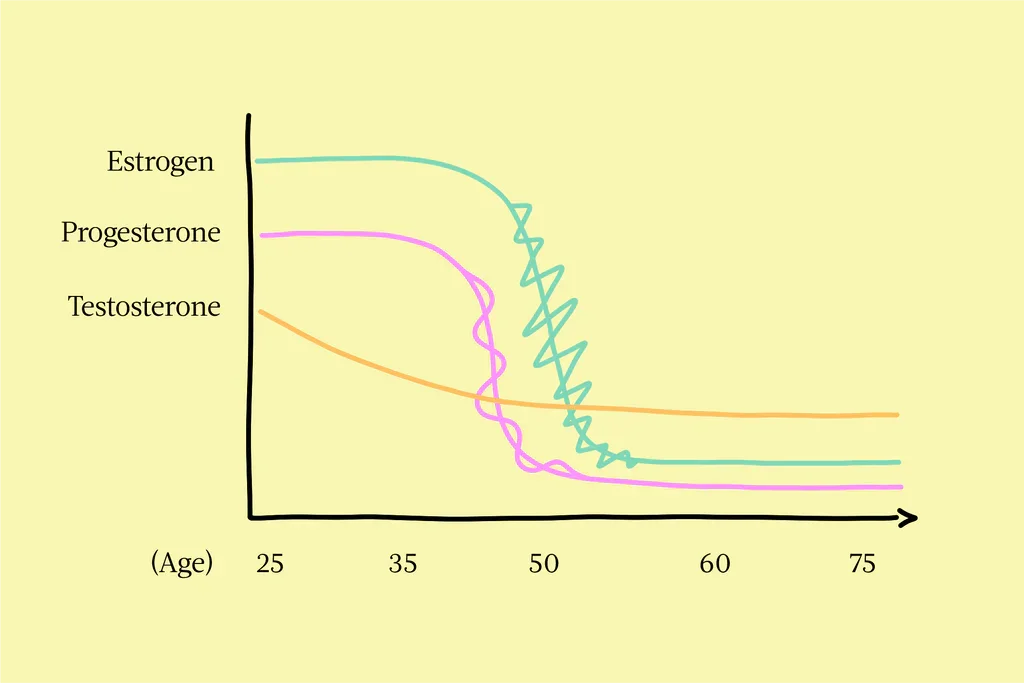
Hormones don’t steadily decline, they fluctuate
Estrogen can spike high one month and drop suddenly the next
Progesterone often declines earlier and more consistently
These shifts affect far more than reproduction. Hormones directly influence:
Brain chemistry
Blood vessels
Inflammation
Nervous system regulation
Gut and liver detox pathways
Which is why headaches are so common during this phase, along with other symptoms.
Why Headaches Increase During Perimenopause
1. Estrogen Fluctuations (Not Just “Low Estrogen”)
Estrogen plays a major role in regulating blood vessels and neurotransmitters in the brain.
During perimenopause, it’s not simply low, it’s unstable.
Rapid rises and falls in estrogen can:
Trigger blood vessel dilation and constriction
Increase sensitivity to pain
Alter serotonin levels (which help regulate headaches)
This is why headaches often show up:
Right before your period
During ovulation
After a month that “felt extra hormonal”
After extra stress
2. Progesterone Decline and Nervous System Tension
Progesterone has a naturally calming effect on the brain and nervous system. As progesterone begins to decline:
The nervous system may become more reactive
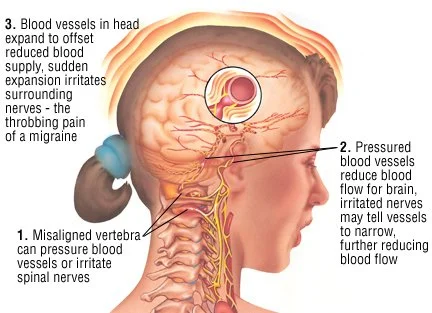
Muscles - especially neck, jaw, and shoulders - may hold more tension
Sleep can become lighter or more disrupted
All of this creates fertile ground for tension headaches and migraines.
3. Blood Sugar Instability
Hormonal changes can make blood sugar regulation more fragile, even in women who “eat well” or “eat clean”.
Blood sugar dips can trigger headaches through:
Stress hormone release (cortisol, adrenaline)
Increased inflammation
Reduced brain fuel
This is why headaches may improve after eating or worsen if meals are delayed or unbalanced.
4. Histamine and Inflammation Sensitivity
Estrogen influences histamine levels in the body.
During perimenopause:
Histamine tolerance may decrease
Mast cells may become more reactive
Inflammatory responses may increase
This can contribute to headaches that:
Come with facial puffiness or sinus pressure
Feel inflammatory rather than strained muscles
Are triggered by certain foods, alcohol, or environmental exposures
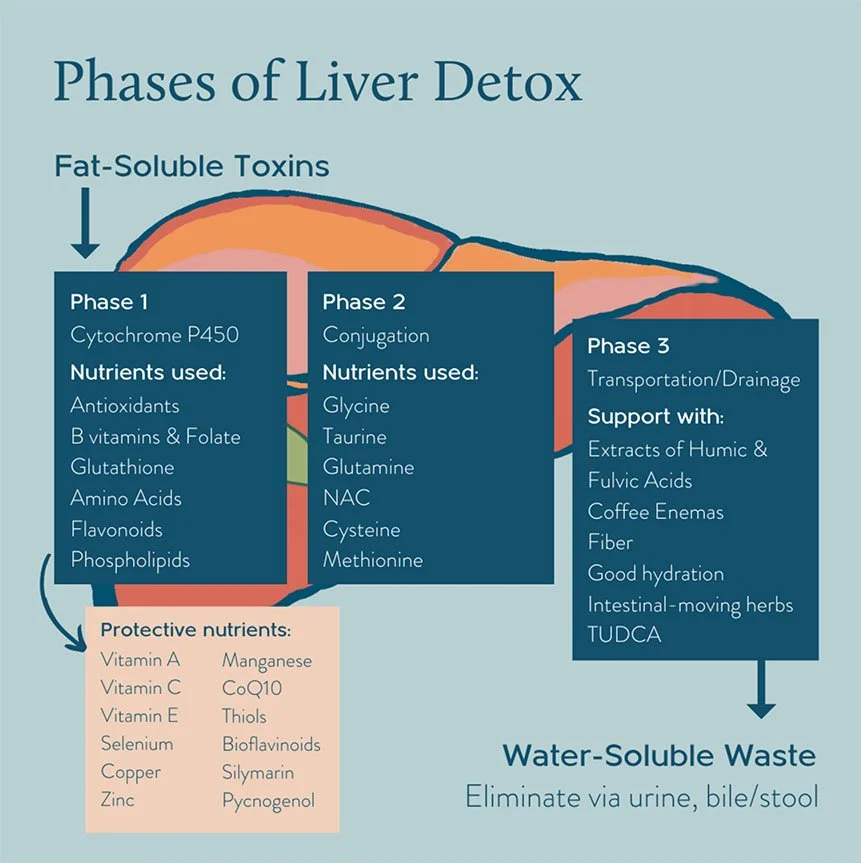
5. Detox and Liver Load
Hormones are metabolized through the liver and gut. If detox pathways are under strain — from stress, constipation, environmental toxins, or inflammation — estrogen metabolites can recirculate rather than exit efficiently.
This can amplify:
Hormone-driven headaches
PMS migraines
Cyclical symptom intensity
A More Supportive Way to Approach Perimenopause Headaches
Instead of asking, “How do I stop the headache?”
A better question is:
“What is my body asking for right now?”
Here are foundational areas that often make a meaningful difference.
1. Support Blood Sugar Stability
This alone can reduce headache frequency for many women.
Helpful daily habits:
Eat protein at every meal
Avoid skipping meals, especially earlier in the day
Pair carbohydrates with fats and protein
Include a balanced snack if headaches tend to hit mid-afternoon
We want nourished bodies, ladies.
2. Prioritize Nervous System Regulation
Perimenopause is a season where the nervous system needs more care.
Gentle supports include:
Consistent sleep and wake times
Morning light exposure
Slow, intentional breathing
Walking, gentle strength training, or yoga
Reducing overstimulation (constant noise, screens, multitasking)
A regulated nervous system can dramatically reduce headache susceptibility.
Smelling pleasant natural fragrances, such as fresh flowers, can help calm the nervous system.
3. Support Digestion and Elimination
Regular bowel movements matter more than many women realize, especially during hormonal transitions.
Simple supports may include:
Adequate hydration
Fiber from whole foods (and natural additions when needed)
Magnesium, particularly glycinate
Supporting bile flow and digestion
When the gut moves well, hormones clear more smoothly and headaches often ease.
4. Reduce Inflammatory Triggers
Many women notice increased sensitivity to:
Highly processed foods
Restaurant meals
Seed oils and additives
Alcohol
This doesn’t mean you have to eat perfectly. It simply means your body may be asking for cleaner, simpler foods more often than before. Our bodies were designed to eat real, whole foods, not flavor enhancers (like MSG), preservatives, sweeteners (like aspartame, high-fructose corn syrup), artificial colors, and thickeners/stabilizers (like xanthan gum, guar gum, carrageenan)
5. Understand Your Headache Pattern
One of the most empowering steps is pattern recognition.
Helpful questions:
Do headaches track with your cycle? (do they come a certain time of your cycle each month)
Do they follow poor sleep or skipped meals?
Do they worsen with constipation or bloating?
Are they associated with neck tension, sinus pressure, or inflammation?
Headaches carry information. Learning their language is powerful.
A Hopeful Truth About Perimenopause Headaches
Perimenopause headaches are not a life sentence.
They are signs of a body in transition, asking for a new level of support.
With the right foundations in place, many women experience:
Fewer headaches
Less intensity
Shorter duration
A greater sense of control and confidence
This phase isn’t about losing your body, it’s about learning how to work with it in a new way.